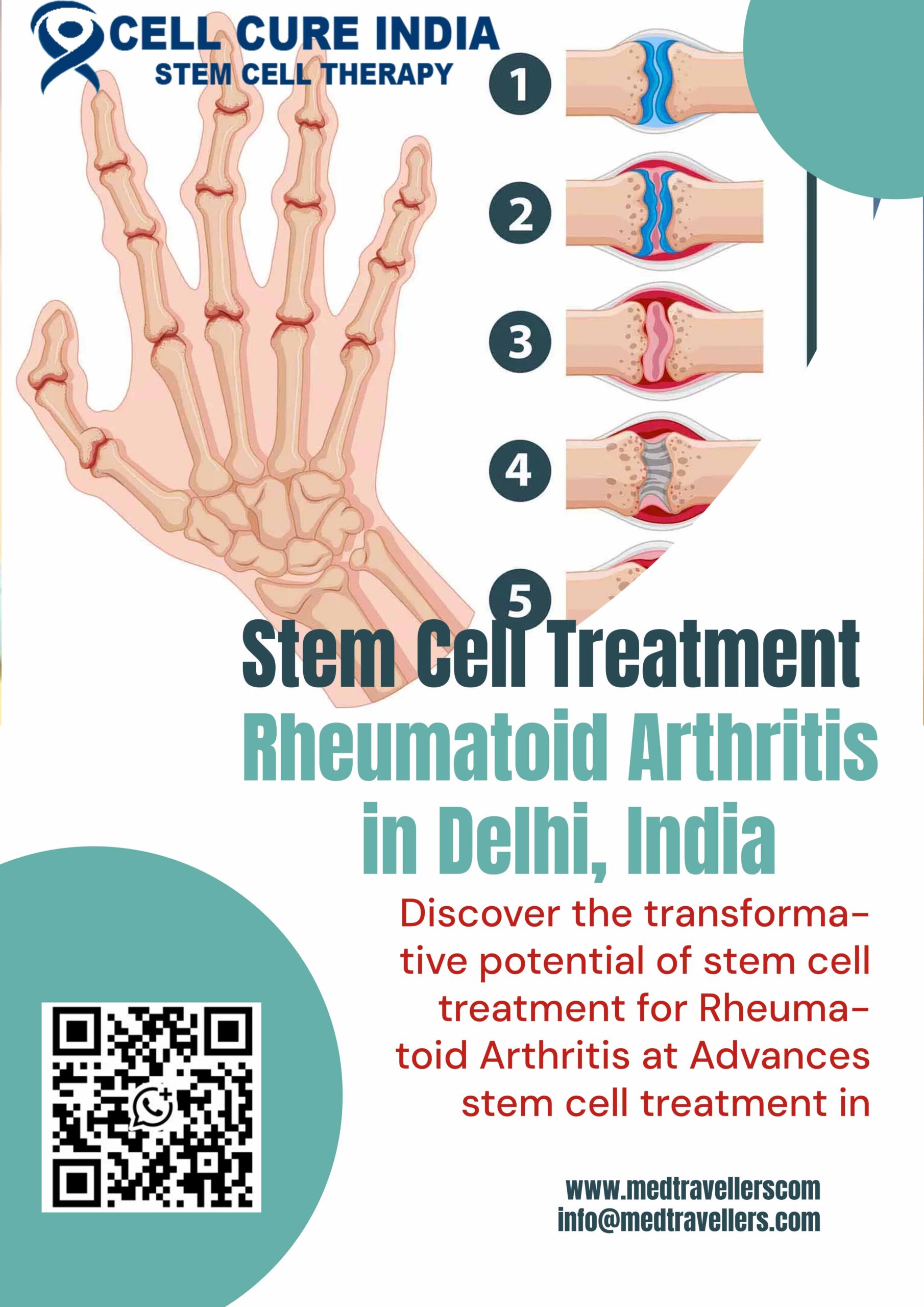
Stem Cell Treatment for Rheumatoid Arthritis in Delhi, India
Rheumatoid Arthritis (RA) is a chronic autoimmune disease characterized by the body’s immune system attacking its own joint tissues. This causes inflammation, swelling, stiffness, and pain in the joints and, if not addressed early, can result in damage and disability. When considering the cause, RA can be distinguished from a normal wear-and-tear form of arthritis in that the inflammation is driven by a faulty immune response wherein antibodies attack healthy tissues. Over time, the inflammation, like that experienced from an acute joint injury, generates the continuing erosion of cartilage and bone and loss of joint function. In some cases, inflammation may affect other organs in the body, including the heart, lungs, and blood vessels.
The early, common presentation of RA is persistent joint stiffness, often first noted in the morning. Without treatment or intervention, the stiffness likely will progress to joint deformities. Patients are often assessed for blood markers associated with RA, such as rheumatoid factor or anti-CCP antibodies; importantly, these are markers demonstrating the involvement of the immune system. Patients often are prescribed medication to avoid discomfort related to inflammation and joint injury. Anti-inflammatory medications, particularly corticosteroids (steroids), are used regularly but rarely slow or stop disease progression when RA is considered resistant to current treatments.
Stem cell therapy for rheumatoid arthritis in India is evolving as a viable and effective treatment option. Mesenchymal stem cells (MSCs) can reset the immune system and alleviate the inflammation and damaged tissues associated with most cases of RA. Based on the time of diagnosis and treatment adoption, stem cell therapy may minimize the damage and support flexibility in the joints, thus avoiding organ involvement and providing incredible improvements in the quality of life for RA patients as well.
Symptoms of Rheumatoid Arthritis
Rheumatoid arthritis typically affects the joints symmetrically throughout the body. That being said, wrists, fingers, knees, feet, and ankles are the places that are affected the most. The symptoms of rheumatoid arthritis include conditions that can be addressed effectively with stem cell treatment for rheumatoid arthritis in India:
- Joint swelling and stiffness
- Joint stiffness in the morning and after repeated sitting
- As the disease progresses, the joints can lose range of motion and get deformed.
- Pain in the chest when breathing (pleurisy)
- Dryness in eyes and mouth (Sjogren syndrome)
- Burning, itching, and discharge from the eyes
- Numbness, tingling, or burning in the hands or feet
- Irritability
- Fatigue
Types of Rheumatoid Arthritis
Rheumatoid Arthritis (RA) is an autoimmune disease where the immune system mistakenly attacks and causes ongoing joint inflammation, pain, and swelling. While the exact cause of RA is not fully understood, recent evidence implicates immune chemicals that are most associated with RA, tumor necrosis factor (TNF) and interleukin-1 (IL-1), as insults to joint health by chronic inflammation and joint damage due to overactivity.
There are two types of RA that are identified in clinical symptoms, imaging, and lab tests, such as blood work; the most important lab marker is rheumatoid factor (RF), an autoantibody in the blood of RA patients.
Rheumatoid Factor Positive (Seropositive RA): Seropositive RA is defined as being in the group of 60-80% of patients with RA who are positive for at least one RF. This autoantibody can be detected in the blood years before any signs or symptoms of RA develop; RA is more common in patients with a family history of RA. In general, seropositive RA is associated with more severe joint inflammation and more long-term joint damage.
Rheumatoid Factor Negative (Seronegative RA): Some RA patients are not positive for RF (seronegative) and yet have RA. Seronegative RA may be milder in some cases; however, like seropositive RA, patients with seronegative RA still will require similar therapies to manage and control symptoms while helping to prevent disease-associated damage over the long term. Diagnosing RA after blood work, X-rays, physical examination, and fully developing the patient’s clinical history provides the lowest chance of misdiagnosing RA.
Ongoing research continues to explore new therapies, including stem cell therapy, which produces promising results in putting immune disease in control.
Causes of Rheumatoid Arthritis
Rheumatoid joint pain happens when your immune system attacks the synovium—the lining of the membranes that shelter your joints.
The resulting inflammation thickens the synovium, which can eventually damage the cartilage and bone within the joint. The ligaments and tendons that secure that joint weaken and lengthen. Over time, the joint loses its shape and alignment.
Doctors don’t know what triggers this process, although a genetic component seems to be a factor. While your genes don’t necessarily cause rheumatoid joint pain, they can make you more susceptible to environmental factors—such as infection with specific viruses and bacteria—that may initiate the disease.
Diagnosis of Rheumatoid Arthritis
Rheumatoid Arthritis (RA) is frequently hard to diagnose because many of its symptoms, such as joint pain, stiffness, and swelling, can mimic several other conditions. While there is no single test that will confirm the diagnosis of RA, a combination of blood tests and imaging studies helps the physician nail down a diagnosis.
Blood tests typically used in diagnosing RA include:
- Erythrocyte Sedimentation Rate (ESR): Tells us about general inflammation in the body in addition to helping us assess symptoms of stiffness, fatigue, and weight loss.
- C-Reactive Protein (CRP): Measures the levels of CRP protein, which tends to rise when there is inflammation.
- Full Blood Count (FBC): Not specific to RA but helpful in ruling out other diseases with similar symptoms.
- Rheumatoid Factor (RF): Identifies antibodies that destroy healthy tissues. RF is not entirely definitive; however, nearly all patients with RA will show their levels of RF are elevated.
- Anti-Cyclic Citrullinated Peptide (anti-CCP): Checks for the presence of anti-CCP antibodies. A positive result in this test very strongly indicates RA and tends to predict more persistent or severe cases of RA.
Imaging studies of joints such as X-ray, ultrasound, or MRI are also performed. These allow doctors to differentiate RA from other forms of arthritis while allowing them to assess the level of joint involvement and monitor the progression of the disease. Early diagnosis of your condition using methods available today is essential to an effective treatment regimen.
Treatment of Rheumatoid Arthritis
Stem cell therapy for rheumatoid arthritis (RA) represents the cutting edge of regenerative medicine, as it can actually repair the damaged tissues and regulate the immune system. RA is a type of chronic autoimmune disease where the body improperly thinks it is against itself and viciously attacks its own joints, creating inflammation, stiffness, and pain. Though traditional treatments usually improve symptoms, they do not actually repair the damage to joints. Stem cells are different from traditional medications because they can self-renew, transform, and differentiate into numerous cell types, giving stem cells several powerful regenerative effects.
Mesenchymal stem cells (MSCs), typically from adipose tissue, bone marrow, or umbilical cord tissues, can reduce inflammation by releasing anti-inflammatory mediators, regenerate cartilage and connective tissues, and activate T regulatory cells that protect against further self-attack. When stem cells are given through an IV line, they are released to travel to damaged areas, regulate immune challenges, and promote damaged tissue to heal.
While treatment is not a permanent “cure,” it does greatly improve a patient’s quality of life by reducing their pain, improving their ability to move around, and slowing the progression of an ongoing disease. Cell Cure India is an organization that provides autologous stem cell treatment (self-derived stem cells) as well as allogeneic stem cell treatment (clinical, properly screened umbilical cord biological products). Patients are advised to stay with us at least three days in VIP accommodations with 24/7 supervision by medical personnel.
FAQs
1. What is Rheumatoid Arthritis (RA)?
RA is a chronic autoimmune disease in which the immune system attacks healthy tissue surrounding the joints. The main symptoms include inflammation, stiffness, swelling, and progressive joint damage leading to decreased mobility.
2. How does stem cell therapy help patients with RA?
Stem cell therapy utilizes mesenchymal stem cells (MSCs) that can repair damaged tissue, reduce inflammation, and modulate the immune system, as well as provide improved range of motion and flexibility of the joints.
3. Is stem cell therapy a cure for RA?
No, stem cell therapy is not a permanent cure for RA. However, it can substantially improve symptoms, slow disease progression, and improve the quality of life for people living with RA.
4. Why Delhi for RA stem cell treatment?
Delhi is home to the Cell Cure India center, which offers advanced care, fully qualified doctors, both autologous and allogeneic stem cell treatments, VIP room treatment for patients, and all-day, every-day concierge service for patients before and after the treatment process.